[MD.PhD.] Why You Must Fast Before a Blood Test (2026)
Why You Must Fast Before a Blood Test: A Laboratory Medicine Specialist’s Complete Guide

Laboratory Medicine, April 13, 2026
Fasting before a blood test is one of the most commonly given — and most commonly ignored — medical instructions. As a Laboratory Medicine Specialist, this guide explains exactly which lab values rise or fall after eating, why fasting is clinically essential for an accurate baseline, and how long you actually need to fast. Understanding this helps you avoid false results that could lead to unnecessary follow-up testing or, worse, a missed diagnosis.
Why fasting matters for blood tests
Every time you eat, your digestive system goes to work — breaking down carbohydrates into glucose, releasing lipids into the bloodstream as chylomicrons, triggering hormonal cascades, and diluting blood components with absorbed fluids. These are entirely normal physiological responses, but they temporarily shift dozens of laboratory values away from your true baseline.
The goal of a health screening panel is to capture your resting metabolic state — what your body looks like when it isn’t actively digesting a meal. This baseline is what reference ranges and clinical decision thresholds are built upon. Testing after a meal introduces unpredictable variability that can mask real disease or create the appearance of abnormality where none exists.
How long should you fast?
| Test category | Recommended fast | Notes |
|---|---|---|
| Standard metabolic panel (glucose, lipids, liver enzymes) | 8–12 hours | Most common requirement; plain water is permitted |
| Fasting plasma glucose / HbA1c | 8 hours minimum | Oral intake other than water invalidates glucose |
| Lipid panel (TG, LDL, HDL, total cholesterol) | 9–12 hours | Triglycerides are the most sensitive; fatty meals extend the effect |
| Insulin / C-peptide | 8–10 hours | Any caloric intake causes significant insulin surge |
| Hormone panels (aldosterone, cortisol) | 8–12 hours + positional rest | Upright posture and time of day also matter |
| Iron / ferritin / TIBC | 8 hours | Dietary iron and inhibitors (calcium, fiber) interfere with serum iron |
Reference ranges and fasting requirements may vary by laboratory and clinical guideline version.
Lab values that rise after eating
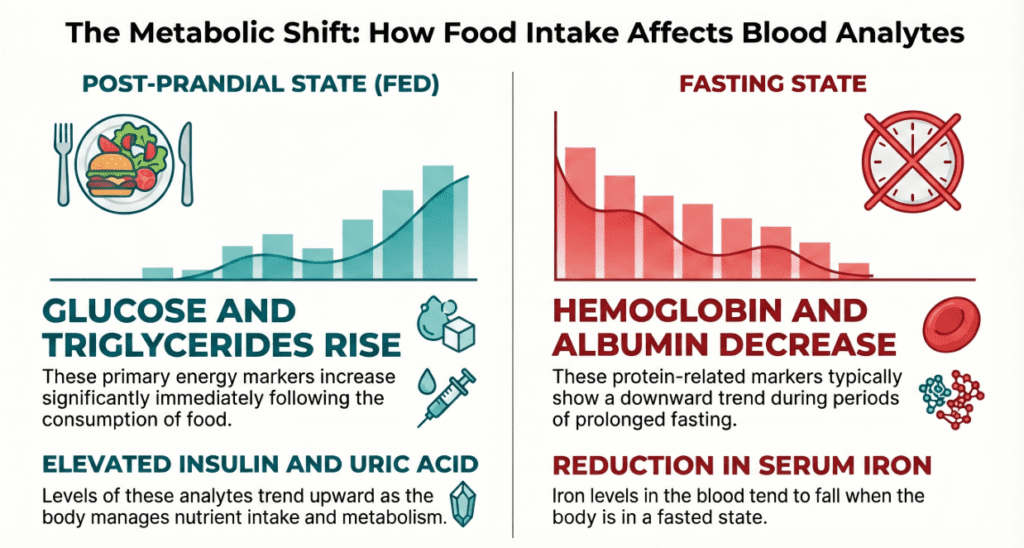
↑ Increased after a meal
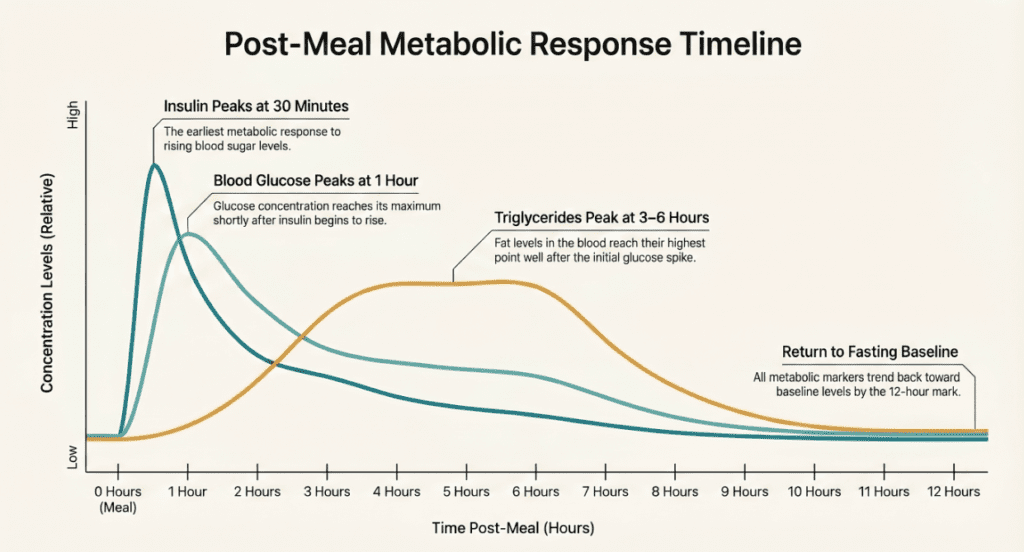
- Glucose — Carbohydrate intake drives blood sugar up; even healthy individuals can reach 140–180 mg/dL at the 1-hour post-meal peak. Fasting glucose is the standard threshold for diabetes screening.
- Triglycerides (TG) — The single most food-sensitive lipid parameter. TG peaks 3–6 hours post-meal and is especially volatile after high-fat foods. This is why fasting is non-negotiable for lipid panels.
- Uric acid — High-protein or purine-rich meals cause transient uric acid elevation; short-term fluctuations are large enough to affect gout diagnosis thresholds.
- Insulin — Rises sharply within 30 minutes of eating. Insulin resistance testing (HOMA-IR) is meaningless without confirmed fasting status.
- LDL cholesterol — Post-meal chylomicrons interfere with the Friedewald equation used to calculate LDL, rendering the result unreliable.
- Aldosterone — Sensitive to dietary sodium, body position, and food timing; always measure at rest, fasted, and in the morning.
- Creatinine — Marginally elevated after large protein meals due to increased muscle creatine turnover and gut absorption of dietary creatine.
Lab values that fall after eating
↓ Decreased after a meal
- Hemoglobin (Hb) & Hematocrit (Hct) — Fluid absorption from food and beverages dilutes blood volume, causing a relative drop. This can mimic borderline anemia in a fed sample.
- Total protein & Albumin — Hemodilution from post-meal fluid shifts lowers protein concentrations, potentially masking true nutritional or hepatic status.
- Serum Iron (Fe) — Multiple dietary components — calcium, polyphenols, high-fiber foods — actively inhibit iron absorption and can suppress serum iron readings. Critical for evaluating iron-deficiency anemia.
- White blood cell count (WBC) — Post-meal leukocyte redistribution (postprandial leukocytosis) has been documented, though direction and magnitude are variable. Fasting sampling removes this confound.
Clinical interpretation at a glance
| Analyte | Fasting reference range | Unit | Sensitivity to food |
|---|---|---|---|
| Fasting plasma glucose | 70–99 | mg/dL | Very high |
| Triglycerides | <150 | mg/dL | Very high |
| LDL cholesterol (calculated) | <100 (optimal) | mg/dL | Moderate–high |
| Total cholesterol | <200 | mg/dL | Moderate |
| HDL cholesterol | ≥40 (M), ≥50 (F) | mg/dL | Low |
| Serum iron | 60–170 (M), 50–170 (F) | µg/dL | Moderate–high |
| Uric acid | 3.5–7.2 (M), 2.6–6.0 (F) | mg/dL | Moderate |
| Fasting insulin | 2–25 | µIU/mL | Extremely high |
Reference ranges vary by laboratory method, reagent, and patient population. Always interpret in context with your physician.
Precautions and common mistakes
Coffee & tea
Black unsweetened coffee causes modest glucose and cortisol fluctuation. Any milk, cream, or sugar breaks the fast entirely. When uncertain, avoid all beverages except plain water.
Medications
Statins, metformin, diuretics, and oral contraceptives all affect lipid, glucose, or electrolyte panels. Do not discontinue medication without physician approval — document it instead.
Exercise
Strenuous exercise within 24 hours raises creatinine, LDH, CK, and AST — enzymes that overlap with cardiac and liver markers. Avoid intense workouts the day before blood draw.
Timing of draw
Certain hormones (cortisol, testosterone, aldosterone) follow circadian rhythms. Morning draws — typically before 9 AM — are the clinical standard for hormone testing.
Hydration
Dehydration concentrates blood components and makes venipuncture harder. Drink 1–2 glasses of plain water before your blood draw unless instructed otherwise.
Self-diagnosis risk
A single abnormal result — even a valid fasting one — should never be used for self-diagnosis. Trend over time, clinical context, and physician interpretation are always required.
A specialist’s perspective
In clinical practice, I frequently receive calls from clinicians puzzled by a triglyceride value of 400 mg/dL in a patient who appeared otherwise healthy. The first question I always ask is: “Was this a fasting sample?” More often than not, the answer is no — and the value normalizes entirely when redrawn under proper fasting conditions.
Triglycerides and glucose are the two analytes I would never interpret without confirmed fasting. For lipid panels specifically, the European Atherosclerosis Society now recommends a minimum 9-hour fast, and some cardiometabolic panels extend this to 12 hours for triglyceride-rich lipoprotein studies. When in doubt, fast longer, drink water, and come in the morning.
Finally, remember that fasting status must be documented in the lab requisition. A value flagged as “non-fasting” should be interpreted — or ideally, repeated — differently than a certified fasting draw. This seemingly administrative detail is one of the most clinically meaningful pieces of metadata attached to a lab result.
Written by a Laboratory Medicine Specialist, MD.PhD.
Board-certified in Clinical Pathology and Laboratory Medicine with over a decade of experience in diagnostic interpretation, quality assurance, and patient education. Subspecialty interest in clinical chemistry and metabolic disease biomarkers.
Why Do Students Who Sit in the Front Perform Better? – MedLab Insight
Some images are generated by AI.
References
- Nordestgaard, B. G., et al. (2016). Fasting is not routinely required for determination of a lipid profile. European Heart Journal, 37(25), 1944–1958. https://doi.org/10.1093/eurheartj/ehw152
- American Diabetes Association. (2024). Standards of Medical Care in Diabetes — Classification and Diagnosis. Diabetes Care, 47(Suppl 1), S20–S42.
- Simundic, A. M., et al. (2018). Joint EFLM-COLABIOCLI recommendation for venous blood sampling. Clinical Chemistry and Laboratory Medicine, 56(12), 2015–2038.
- Riley, R. S., & McPherson, R. A. (2017). Basic examination of urine. In Henry’s Clinical Diagnosis and Management by Laboratory Methods (23rd ed.). Elsevier.
- Mayo Clinic Laboratories. (2025). Test Catalog: Fasting requirements for common analytes. Retrieved from https://www.mayocliniclabs.com
- UpToDate. (2025). Patient education: Blood tests (Beyond the Basics). Wolters Kluwer.
- Patient education: Blood donation (Beyond the Basics) – UpToDate
